Trauma’s Labyrinth:
Reflections of a Wounded Healer
Essays

Recipient of 2022 Bronze
Living Now Book Award
Synopsis:
Trauma can feel like a labyrinth, twisting on itself like a maze of despair, without end or exit. This seems particularly true in today’s chaotic world of pandemics, climate change, social conflict, and systemic violence. Increasingly, the conditions of the larger world aggravate, if not cause, the traumas in our individual lives.
However, as Laura K. Kerr explores in this wide-ranging collection of essays, not only can we heal from trauma, but we can use it as an opportunity for growth and transformation, changing ourselves and the world for the better. Drawing from her experiences as researcher, trauma survivor, and psychotherapist, she examines various causes of trauma, details how to understand and treat trauma’s effects, and explores the role society plays in activating traumatic defenses. Despite the weightiness of the topic, Dr. Kerr brings hope for lasting, positive change.
As Dr. Kerr shows, the key lies in removing rigid divides, like those between wounded and healer, self and society. When they are integrated, healing becomes transformative and enduring—not only for ourselves but for the increasingly traumatized world in which we live.


Other essays from the original online project:
Trauma’s Labyrinth is derived from my former online project of the same name. Through much revision and editing, the book contains about a third of the original material. The essays included were selected because of their importance for recovery and relevance to present world conditions. Some of the original essays not in the book are archived below.
The Hero and Heroine Archetypes in Action
Challenging times bring forth the best and worst in humanity. In our darkest moments, many of us benefit from an image of our better selves or someone we admire who can inspire us to continue the good fight with hope, if not also heroism. But what...
Trickster Will Have Its Way
The Trickster has been depicted as both mythical figure and archetype — what Carl Jung identified as instinctual schemas guiding behavior that serve both individual and social development. As archetype, Trickster is a masterful, yet...
What is the function of the brain?
Based on her ethnographic study of psychiatric residency programs, anthropologist T.M. Luhrmann concluded psychiatry is “of two minds,” much like the Axis I and Axis II diagnoses organizing the Diagnostic and Statistical Manual of Mental...
At Times Hypocrisy is the Best We Can Do
In My Green Manifesto, nature writer David Gessner shared of paddling down the Charles River with environmentalist Dan Driscoll as Driscoll spoke of the need for hypocrites in the green movement: “We nature lovers are hypocrites of course,”...
Trauma’s Imaginal Worlds
Few people pass from birth to death without intimate knowledge of trauma’s capacity to alter the landscape of their lives. So many experiences are traumatizing: war, rape, death of a loved one, car accidents, hurricanes, bullying, scapegoating,...
Addressing the Shadow Side of Creativity
Designer Charles Eames warned of an emerging cultural obsession with the creative process: Recent years have shown a growing preoccupation with the circumstances surrounding the creative act and a search for the ingredients that promote...
Too Stressed to Meditate?
Buddhist psychology claims there are three primary emotions or sensations — pleasant, painful, and neutral. Arising from these primary emotions are our reactions to them, the so-called secondary emotions. For example, we might...
The Eternal Marriage
My husband and I have been together almost 36 years, 32 of them married. We know couples past the 50-year point. Some like to trump our landmark. “Pshaw. Newlyweds.” But in a nation where half of marriages end in divorce, and about half the...
Love and the Split Self
In the movie Take This Waltz, a young Canadian woman, Margot, is happily married although not excited about her life. Her work doesn’t fulfill her. She designs brochures but would rather be a “real” writer. She describes herself...
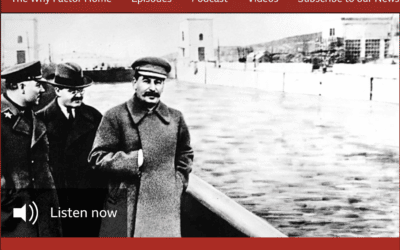
BBC’s “The Why Factor”: On Cultural Memory
BBC's The Why Factor has a short podcast on trauma well worth your time (18 minutes). Cultural Memory explores how societies respond collectively to traumatic memories of war and extreme human rights violations, which too often...
Trauma-Informed Psychotherapy Puts the Body – and Love – Back in Mental Healthcare
For the past 50 years, psychotherapy took a back seat to biomedical psychiatry, largely due to reliance on medications for the treatment of mental disorders. Yet clinical evidence increasingly points to chronic, unresolved traumatic stress as a...
A Sensorimotor Approach to Becoming Indigenous (and Healing Trauma)
While hiking among the hoodoos in Bryce Canyon National Park, I learned the Paiutes Indians called these majestic rock pillars the Legend People who coyote trickster turned to stone because of their evil ways. Looking out on Bryce Canyon, thinking...

laura k. kerr, phd
Mental Health Scholar & Author
The purpose of life is to live it, to taste experience to the utmost, to reach out eagerly and without fear for newer and richer experience.
—Eleanor Roosevelt